Unresectable locally recurrent breast cancers (LRBCs) lead to life-threatening situations and a tremendous loss of quality of life. Most patients have received radiotherapy (RT) during primary treatment and re-irradiation (re-RT) using standard doses might be denied due to the risk of unacceptable cumulative toxicity. Therefore, an effective tumor control is often abandoned.
Mild hyperthermia (39–43 °C), allows for significant reductions in re-RT dose and effective tumor responses with acceptable toxicity even after heavy pretreatment. More than 280 patients have been treated with superficial hyperthermia by water-filtered infrared A (wIRA-HT), which can cover even large lesions. Hyperthermia was immediately followed by hypofractionated re-RT of 5×4 Gy, once a week.
Evaluating 201 patients, overall response rate was 94%. 170 patients with macroscopic LRBC were stratified into 4 size classes (rClasses), and detailed response rates are presented. Accordingly, response rates of 31 patients with microscopic disease after resection of LRBC are communicated.
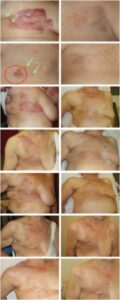
RT-related acute and late toxicity was limited to grades 1 and 2. Due to this low toxicity, re-recurrences after CR and new local progression after PR could be re-treated using the same treatment schedule. Real-time thermographic and visual controls have allowed to almost exclude the risk of thermal skin damage.
Unresectable locally recurrent breast cancers (LRBCs) lead to life-threatening situations and a tremendous loss of quality of life. Most patients have received radiotherapy (RT) during primary treatment and re-irradiation (re-RT) using standard doses might be denied due to the risk of unacceptable cumulative toxicity. Therefore, an effective tumor control is often abandoned.
Mild hyperthermia (39–43 °C), allows for significant reductions in re-RT dose and effective tumor responses with acceptable toxicity even after heavy pretreatment. More than 280 patients have been treated with superficial hyperthermia by water-filtered infrared A (wIRA-HT), which can cover even large lesions. Hyperthermia was immediately followed by hypofractionated re-RT of 5×4 Gy, once a week.
Evaluating 201 patients, overall response rate was 94%. 170 patients with macroscopic LRBC were stratified into 4 size classes (rClasses), and detailed response rates are presented. Accordingly, response rates of 31 patients with microscopic disease after resection of LRBC are communicated.
RT-related acute and late toxicity was limited to grades 1 and 2. Due to this low toxicity, re-recurrences after CR and new local progression after PR could be re-treated using the same treatment schedule. Real-time thermographic and visual controls have allowed to almost exclude the risk of thermal skin damage.

Oplus_131072
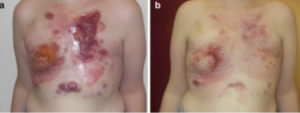
Size classification for locally recurrent breast cancer, as suggested by Notter et al. (modified from [4])
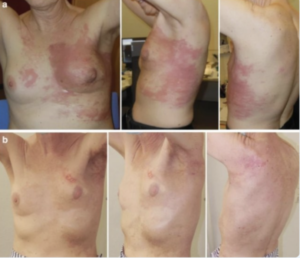
Full size image 6.2.1 Basic Characteristics of the Patients In the intermediate analysis, 170 patients presented with macroscopic disease and 31 patients with microscopic disease. Most patients were heavily pretreated and sent to thermography-controlled wIRA-hyperthermia since no other therapeutic option remained. All patients had previously received radiotherapy, with 116 patients having received more than 2 systemic chemotherapies. Of the patients with macroscopic disease, 141 (83%) had large-sized tumors (rClass II–IV), 49 of whom had 2 or more regions to be treated. Poor prognostic factors were prominent in these patients: 50 patients (25%) presented with triple-negative breast cancer, 115 patients (57%) presented with inflammatory LRBC (lymphangiosis carcinomatosa), and 70 patients (35%) with ulcerating lesions. More than half of the patients with macroscopic disease presented with additional distant metastasis, which is the decisive factor for limited life expectancy. However, effective control of local tumor growth is crucial, even for patients with a life expectancy of just a few months, in order to achieve a satisfying palliative effect, and to improve the quality of life during the remaining lifetime.
6.2.2 Treatment Schedule The basic treatment protocol was thermography-controlled, superficial wIRA-hyperthermia directly followed by hypofractionated re-irradiation of 5 × 4 Gy, once a week, as introduced by Notter et al. [6]. The total re-irradiation dose of 20 Gy is the lowest RT dose ever applied in a protocol aiming for effective tumor control. Since wIRA-HT works with a contact-free energy input, the treatment allows the patient to stay in a comfortable position (see Fig. 6.2a–c). Automatic control of the maximum surface temperature between 42 °C and 43 °C achieves effective hyperthermic temperatures >39 °C up to a depth of approximately 25 mm (Thomsen et al.; see Chap. 5) and overheating leading to thermal skin damage can be avoided. The time interval between HT and RT is 39 °C up to a depth of approx. 30–40 mm. However, the MW technique has considerable limitations as the treatment of large-sized diffuse tumor spread cannot be covered by one applicator, especially in the case of heterogeneous body contours. With ulcerating lesions, the applicator contact may be uncomfortable and painful. In addition, the incidence of thermal skin damage is high [3].
6.2 Patients and Treatments So far, tumor response and local control have been documented in 280 patients presenting with LRBC in pre-irradiated sites and treated with thermography-controlled, superficial wIRA-HT. In 2020, an intermediate analysis of the outcome data of 201 patients was published [4]. Since tumor size has been described as being the most significant prognostic factor [5], the evaluation has been stratified into 4 size classes of macroscopic disease, ranging from tumors 39 °C up to a depth of approximately 25 mm (Thomsen et al.; see Chap. 5) and overheating leading to thermal skin damage can be avoided. The time interval between HT and RT is 39 °C up to a depth of approx. 30–40 mm. However, the MW technique has considerable limitations as the treatment of large-sized diffuse tumor spread cannot be covered by one applicator, especially in the case of heterogeneous body contours. With ulcerating lesions, the applicator contact may be uncomfortable and painful. In addition, the incidence of thermal skin damage is high [3].
6.2 Patients and Treatments So far, tumor response and local control have been documented in 280 patients presenting with LRBC in pre-irradiated sites and treated with thermography-controlled, superficial wIRA-HT. In 2020, an intermediate analysis of the outcome data of 201 patients was published [4]. Since tumor size has been described as being the most significant prognostic factor [5], the evaluation has been stratified into 4 size classes of macroscopic disease, ranging from tumors 39 °C up to a depth of approximately 25 mm (Thomsen et al.; see Chap. 5) and overheating leading to thermal skin damage can be avoided. The time interval between HT and RT is Oplus_131072[/caption]



